Download Products Flyer
What is sepsis?
Sepsis is a complication caused by the body’s overwhelming and life-threatening response to an infection, which can lead to tissue damage, organ failure, and death.
What causes sepsis?
Sepsis is always triggered by an infection. Sepsis occurs as a result of infections acquired both in the community and in hospitals and other health care facilities. The majority of cases are caused by infections we all know about: pneumonia, urinary tract infections, skin infections like cellulitis and infections in the abdomen (such as appendicitis). Invasive medical procedures like the insertion of a catheter into a blood vessel can also introduce bacteria into the blood and trigger sepsis.
Normally, when we suffer a minor cut, the area around the injury swells and becomes hot and red. This is the immune system in action. To fight any infection and to form a blood clot to stop bleeding, the body must get white blood cells and platelets into the tissues surrounding the cut. The body does this through inflammation, which is managed by the immune system. The blood vessels swell to allow more blood to flow, become leaky so that the infection-fighting cells and clotting factors can get out of the blood vessels and into the tissues where they’re needed, and we see the typical hot, red swelling.
Sepsis is best thought of as this process in overdrive: inflammation is no longer localized to the “cut”, but is now widespread affecting all of the body’s organs and tissues. The body ́s defense and immune system go into overdrive, leading to widespread inflammation, poor perfusion, organ failure and septic shock. Most types of microbes can cause sepsis, including bacteria, fungi, viruses and parasites such as those causing malaria. Bacteria are by far the most common culprit, but it is important to understand that viral infections with seasonal influenza viruses, the Dengue and Ebola viruses may also progress to acute organ dysfunction and result in death from multiple organ failure and septic shock.
Source: World Sepsis Day
Common symptoms of sepsis
There is no single sign or symptom of sepsis. It is, rather, a combination of symptoms. Since sepsis is the result of an infection, symptoms can include infection signs (diarrhea, vomiting, sore throat, etc.), as well as ANY of the symptoms below:
- Shivering, fever, or very cold
- Extreme pain or discomfort
- Clammy or sweaty skin
- Confusion or disorientation
- Shortness of breath
- High heart rate
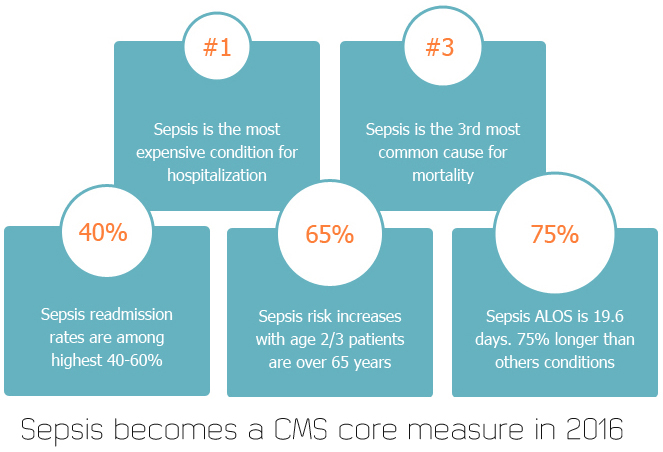
Sepsis facts
How is sepsis diagnosed?
The presence of sepsis is indicated by blood tests showing particularly high or low white blood cell counts. The causative agent is determined by blood culture.
In some cases the doctor may order imaging studies to rule out pneumonia, or to determine whether the sepsis has developed from a ruptured appendix or other leakage from the digestive tract into the abdomen.
Identifying the specific causative agent ultimately determines how sepsis is treated. However, time is of the essence, so a broad-spectrum antibiotic or multiple antibiotics will be administered until blood cultures reveal the culprit and treatment can be made specific to the organism. Intravenous antibiotic therapy is usually necessary and is administered in the hospital. The patient’s chances of survival are increased by rapid admission to an intensive care unit followed by aggressive treatment with antibiotics.
How many people get sepsis?
Sepsis is a global health problem that carries a high risk of death. A recent global assessment of the mortality rate of patients with sepsis treated in an intensive care unit found that over one third of these patients died without leaving hospital. Sepsis remains the primary cause of death from infection despite advances in modern medicine, such as vaccines, antibiotics and acute care. In the developing world sepsis accounts for 60-80% of lost lives per year, affecting more than 6 million newborns and children annually and over 100,000 women contract sepsis in the course of pregnancy and childbirth. In all countries where data on hospitalization for sepsis are available the number of cases has increased steadily.
The US Center for Disease Control’s National Center for Health Statistics estimates that, based upon information collected for billing purposes, the number of times people were in the hospital with sepsis increased from 621,000 in the year 2000 to 1,141,000 in 2008. The number of hospital admissions for sepsis following healthcare-associated as well as community-acquired infections increased up to three-fold over the last decade. In comparison hospital admissions for stroke and myocardial infarction remained stable over the same period.
The number of deaths from sepsis in the U.S increased from 154,159 in 2000 to 207,427 in 2007 and the numbers of hospitalizations with sepsis have overtaken those for myocardial infarction. In the U.S., sepsis accounts for far more deaths than the number of deaths from prostate cancer, breast cancer and AIDS combined.
The number of hospital-treated sepsis cases in resource rich countries may be up to 7-fold higher because it relies on use of administrative data to identify sepsis patients which likely underestimates the true incidence rate based on clinical assessment or chart review. The reason for the rise in sepsis cases is likely due to a combination of factors, including poor socioeconomic conditions, increased awareness and tracking of the condition, an aging population, with more chronic diseases, an upsurge in major surgical interventions and invasive procedures, broader use of immuno-suppressive and chemotherapeutic agents as well as the spread of antibiotic-resistant organisms.
Source: World Sepsis Day
What is the economic cost of sepsis?
Early identification and treatment of sepsis will have tremendous economic benefits, totally apart from saving lives and reducing the negative impacts of sepsis. Treatment for sepsis often involves a prolonged stay in the intensive care unit and complex therapies, which incur high costs. The Agency for Healthcare Research and Quality lists sepsis as the most expensive condition treated in U.S. hospitals, costing more than $20 billion in 2011 increasing on average annually by 11.9%.
It has been estimated that if the U.S. as a whole achieved earlier sepsis identification and evidenced based treatment, there would be 92,000 fewer deaths annually, 1.25 million fewer hospital days annually, and reductions in hospital expenditures of over $1.5 billion.
The costs related to long-term impacts of sepsis have not been quantified but are likely very substantial, including subsequent medical care: the true fiscal burden, considering delayed return to work, the need for families to adjust lifestyles to support, and rehabilitation cost is likely to be huge.
It has been estimated that if the U.S. as a whole achieved earlier sepsis identification and evidenced based treatment, there would be 92,000 fewer deaths annually, 1.25 million fewer hospital days annually, and reductions in hospital expenditures of over $1.5 billion.
The costs related to long-term impacts of sepsis have not been quantified but are likely very substantial, including subsequent medical care: the true fiscal burden, considering delayed return to work, the need for families to adjust lifestyles to support, and rehabilitation cost is likely to be huge.
Who can get sepsis?
Sepsis does not discriminate!
It affects all age groups and is not respectful of lifestyle choices. Vulnerable groups such as new born babies, small children and the elderly are most at risk, as are those with chronic disease and weakened immune systems. It is not a disease confined to healthcare settings, though most patients with established sepsis will be cared for in hospital. Age, sex, and race or ethnic group can all influence the incidence of severe sepsis, which is higher in infants and elderly persons than in other age groups, higher in males than in females, and higher in blacks than in whites. People with chronic illnesses, such as diabetes, cancer, AIDS, kidney or liver disease, are also at increased risk, as are pregnant women and those who have experienced a severe burn or physical injury.
What is the emergency care for sepsis?
Sepsis is an emergency ans must be treated like one. The patient requires immediate medical attention in a hospital with an intensive care unit. His or her chances of survival depend to a large extent on receiving successful treatment for the infection that led to sepsis, including broad-range antibiotics and any other treatment necessary to eliminate the cause of infection. This treatment must also be supported by suitable steps to stabilize blood circulation, like infusions and medicine.
Every minute counts!
• Give high flow oxygen (via non-rebreather mask)
• Take blood cultures
• Give IV antibiotics
• Start IV fluid resuscitation
• Check hemoglobin and lactate Monitor hourly urine output accurately
Source: World Sepsis Day
What is the prognosis with sepsis?
The prognosis of patients with sepsis is related to the severity or stage of sepsis as well as to the underlying health status of the patient. For example, patients with sepsis and no ongoing sign of organ failure at the time of diagnosis have about a 15%-30% chance of death. Patients with severe sepsis or septic shock have a mortality (death) rate of about 40%-60%, with the elderly having the highest death rates. Newborns and pediatric patients with sepsis have about a 9%-36% mortality rate. Investigators have developed a scoring system (MEDS score) based on the patient’s symptoms to estimate prognosis.
Source: Medicinenet
What are the stages of sepsis?
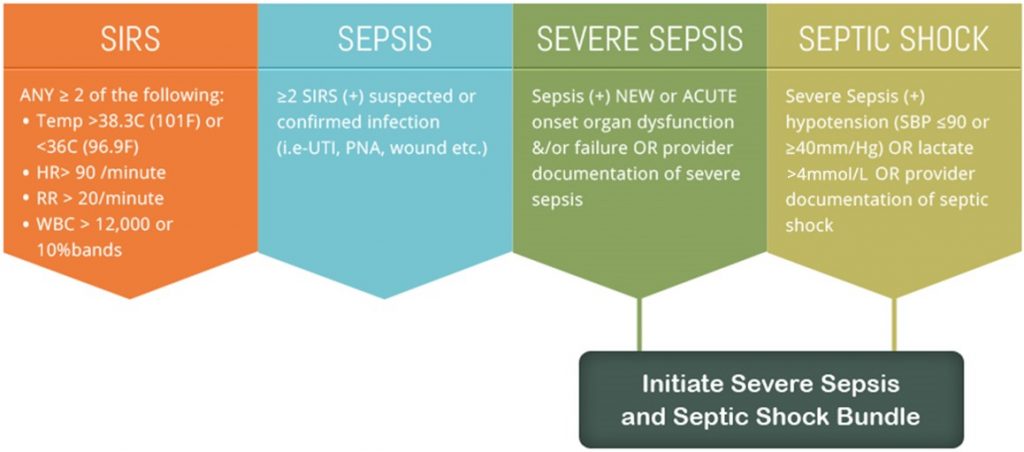
CMS Core Measures for sepsis
SEVERE SEPSIS AND SEPTIC SHOCK: MANAGEMENT BUNDLE MEASURE (NQF #0500)
The Centers for Medicare & Medicaid Services (CMS) now require hospitals participating in Inpatient Quality Reporting (IQR) Program to collect data for the Severe Sepsis and Septic Shock: Management Bundle Measure (NQF #0500).5 With the implementation of this measure, CMS will be able to gauge if care of severe sepsis and septic shock patients is improving. Compliance with this measure will determine payment starting Fiscal Year 2017.5
Download CMS Core Measures for Sepsis
- What is sepsis?
- What causes sepsis?
- Common symptoms of sepsis
- Sepsis facts
- How is sepsis diagnosed?
- How many people get sepsis?
- What is the economic cost of Sepsis?
- Who can get sepsis?
- What is the emergency care for Sepsis?
- What is the prognosis with sepsis?
- What are the stages of sepsis?
- CMS Core Measures for sepsis
